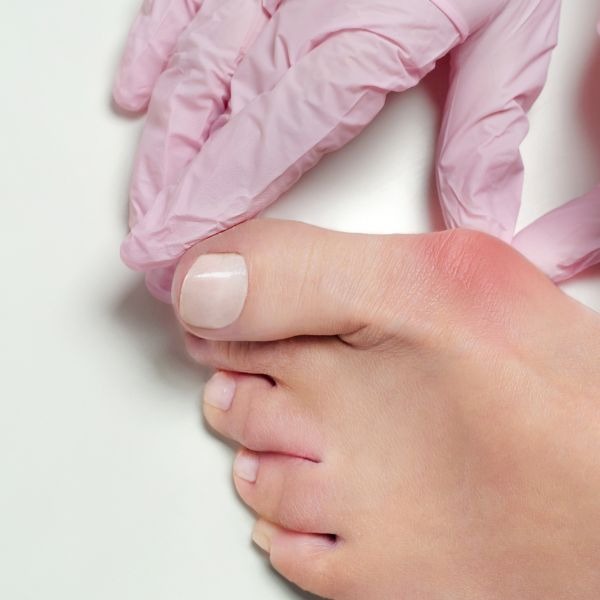
Gentle signs of trouble under the skin
Foot care starts with honest notes from the feet. An ingrown callus on foot may begin as a stubborn patch of thick skin that refuses to soften after a shower. It often brings a dull ache when pressure lands on the pad or edge of the sole. The skin may appear slightly ingrown callus on foot red or irritated, and wearing tight shoes makes the sting sharper. People notice that walking after a long day feels odd, as if the foot is trying to tell a story it cannot finish. Early awareness can stop a bigger problem from budding.
Why pressure turns rough and painful
When the skin thickens, it acts like a shield against constant rubbing. The natural response to friction can trap a bit of skin in the toe crease or along the arch. Pain may spike with steps that require toe push-off or when standing on hard floors. The painful callus on foot treatment phrase painful callus on foot treatment should start with simple changes: wider shoes, cushioned insoles, and regular, gentle exfoliation. If the zone hardens and becomes tender, the clock is ticking toward a sharper problem unless care is stepped up.
Everyday habits that help soften the texture
Regular soaks help, but the real trick lies in routine. Soak the feet in warm water with a touch of Epsom salt for ten to fifteen minutes. Then file the surface with a pumice stone or a gentle emery board, taking care not to remove too much skin at once. A soft, non-medicated cream applied after a soak keeps moisture in and reduces cracking. Keep footwear roomy and choose socks that wick away sweat. These small acts, repeated weekly, curb the stubborn build-up and reduce discomfort.
When to seek professional guidance
If the skin thickens again after home care, or if a painful callus on foot treatment seems stuck, a podiatrist can help. A clinician can assess whether the area harbours a tiny corn, a cracked callus, or an underlying issue such as a toe deformity or nerve sensitivity. Medical care might include precise trimming, padding for pressure relief, or a custom orthotic. Even subtle changes in gait can trigger recurring problems, so an expert eye often spot patterns that home routines miss and tailor a plan accordingly.
Tools and tips for safer self-care
Choose a foot file designed for diabetic-safe use if numbness or circulation concerns exist. Always keep tools clean and dry, and avoid sharp objects that could cut skin. Hydration matters; a light oil or balm keeps the skin supple after filing. Mattress-like slippers, soft laces, and break-in time for new footwear all help. A daily routine built on restraint—short steps, gentle pressure, and mindful posture—can prevent the cycle of thick skin from returning, letting toes move with less friction and more comfort.
Conclusion
Foot comfort grows from listening to the body and treating warnings as data. If a patch reappears, map its location and note what shoes or activities trigger it. Keep a simple diary of footwear changes and shoe sizes, and adjust as needed. The aim is not a single fix but a steady, practical plan. With patience, the foot relearns to tolerate everyday wear, and the old ache eases into a faint reminder rather than a loud indictment. Consistency beats sudden cures every time.